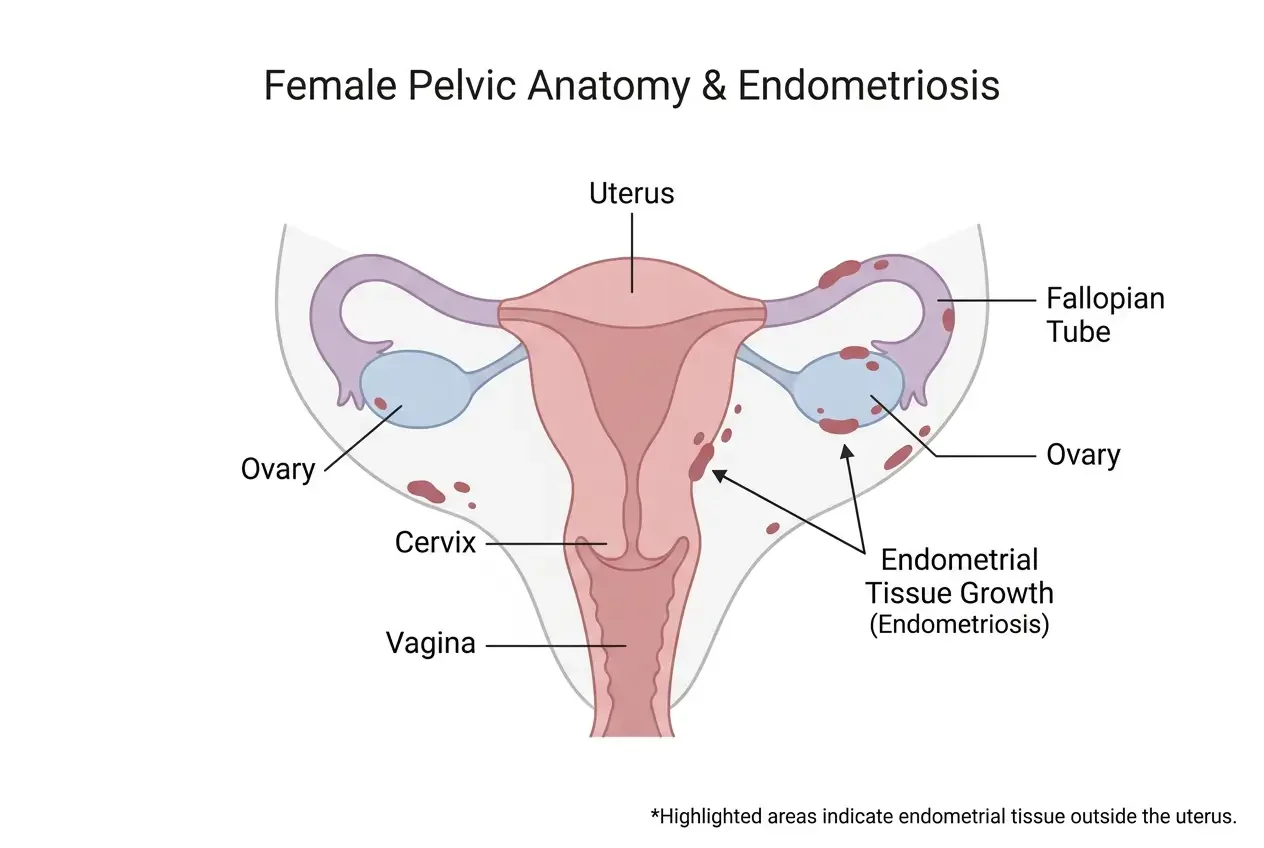
How to Relieve Pelvic Pain from Endometriosis
If you have endometriosis, you already know the pain is real. You've probably also figured out that the standard conversation around endo — focused almost entirely on the uterus, hormones, and surgery — doesn't fully explain what you're experiencing in your body every day.
That's because research is catching up to what many in the endo community have been saying for years: endometriosis isn't just a gynecological condition. It's a systemic inflammatory disease, and understanding it that way changes what management and relief can actually look like.
This post covers what's driving pelvic pain from endometriosis, why certain daily habits make it worse, and practical approaches that can genuinely help.
Endometriosis Is a Whole-Body Inflammatory Disease
For a long time, endometriosis was treated as a localized problem — find the lesions, remove them, done. But growing research is reframing it as a chronic, systemic inflammatory condition that affects immune function, the nervous system, gut health, and more.
A 2025 large-scale study found that people with endometriosis had roughly twice the odds of being diagnosed with an autoimmune condition — such as rheumatoid arthritis, lupus, or Hashimoto's disease — compared to those without it. That's not a coincidence. It reflects shared mechanisms: chronic inflammation, dysregulated immune activity, and a body that is responding systemically, not just locally.
This matters for how you think about managing your symptoms. Targeting lesions alone often isn't enough — and the research increasingly supports a whole-body approach that addresses inflammation, the nervous system, the gut, and daily physical environment alongside any medical treatment.
Why Sitting Can Amplify Pelvic Pain from Endometriosis
One thing that doesn't get enough attention in the endo conversation is how much prolonged sitting contributes to daily pain levels.
Standard chairs direct pressure straight into the tailbone, perineum, and pelvic floor — areas that are often already inflamed in people with endo. When pelvic tissue is sensitized and you're sitting for hours at a desk, in a car, or on the couch, that sustained pressure can cause pain to build significantly over the course of a day even if you started out feeling manageable.
This doesn't get mentioned much, but for a lot of people with endo it's one of the most consistent daily triggers. Reducing that pressure doesn't address the underlying disease — but it can meaningfully reduce one of the things making every day harder.
What Actually Helps with Pelvic Pain from Endometriosis
Managing endo well usually takes a multi-layered approach. Research supports a number of strategies — not as replacements for medical care, but as meaningful complements to it. Here's what has the most evidence and the most real-world impact.
1. Reducing Systemic Inflammation Through Nutrition
Because endometriosis is rooted in chronic inflammation, what you eat can genuinely affect how your symptoms behave. An anti-inflammatory approach — reducing processed foods, refined sugar, alcohol, and red meat while increasing omega-3s, fiber, and colorful vegetables — can shift the inflammatory environment your body is operating in.
Nutritional therapist Katie Edmonds, author of Heal Endo, has done some of the most practical and research-grounded work in this area specifically for endo. Her framework goes well beyond generic dietary advice and addresses the specific inflammatory mechanisms involved. If this is an area you want to explore, healendo.com is a strong starting point.
2. Pelvic Floor Physical Therapy
Endometriosis frequently causes the pelvic floor muscles to become hypertonic — meaning chronically tight — as the body braces around pain. A pelvic floor physical therapist can assess how your specific body is responding to your particular experience of endo, and use manual therapy, breathing work, and targeted exercises to reduce that tension.
This isn't about diagnosing or treating endometriosis itself — it's about addressing how your pelvic floor has adapted to living with it. For many people with endo, this makes a significant difference in day-to-day function and pain levels.
3. Addressing Sitting Pressure
For people who experience chronic pelvic pain with endometriosis, the surface of your sitting area matters a lot. Most cushions just add padding — which still places pressure directly on the tailbone, perineum, and pelvic floor. That's not relief, it's just softer pressure on already inflamed tissue.
The Twin Cheeks cushion works differently. It has two independent foam panels that support the fleshy part of your buttocks, with an open channel running down the center. Your tailbone, perineum, and the pelvic floor tissue beneath you sit completely suspended in that channel — no contact, no compression. Pressure is fully redirected away from the areas that hurt most.
The panels attach with heavy-duty Velcro and adjust to your body width, so the fit is personal. It also folds in half for easy transport — so it goes with you to the office, to appointments, on road trips, wherever you need it. It's handmade to order in Colorado and Georgia, and comes in multiple firmness levels based on your body weight.
People managing endometriosis are using it and have found it makes a meaningful difference for getting through a workday, sitting through appointments, or simply being able to sit on the couch without bracing.
Reducing one of the most consistent daily pain triggers is worth a lot when you're managing something chronic.
Shop the Twin Cheeks Cushion →
4. Nervous System Support
Chronic pain keeps the nervous system in a state of heightened alert, which in turn amplifies how pain signals are processed. This isn't about minimizing what you're experiencing — it's about understanding that the nervous system becomes part of the pain cycle, and working with it is part of managing endo.
Practices that support nervous system regulation — breathwork, gentle movement, endo-informed yoga, time in nature, or somatic-based approaches — have real physiological effects on how pain is experienced. This is an area where the endo community has developed a lot of practical wisdom, and it's worth exploring alongside any medical treatment.
5. Working Toward Remission, Not Just Symptom Management
The current language in the endo community — increasingly supported by research — is that while there is no known cure, remission is a real and achievable goal for many people. That shift in framing matters because it moves the conversation from just managing flares to actively reducing the conditions that allow endo to drive symptoms.
That typically means combining appropriate medical care (including, when relevant, excision surgery with a specialist) with the whole-body strategies above. Katie Edmonds' work and the broader integrative endo community are valuable resources for navigating this.
Living with Endo: You Already Know It's More Than a Uterine Issue
If you've been managing endometriosis for any length of time, you've probably already figured out that the standard story doesn't capture the full picture. The research is finally catching up — and the more it does, the more it validates the whole-body, integrative approach that many in the endo community have been advocating for years.
Managing pelvic pain from endo is rarely about finding the one thing that fixes it. It's about building a toolkit — medical, nutritional, physical, nervous system — that reduces the overall inflammatory burden and helps your body function better day to day.
If pelvic pain is one of your consistent daily triggers, that's one of the more solvable pieces of the puzzle, and it's a reasonable place to start.
Stay ahead with the latest pelvic pain research, resources, and tips — delivered straight to your inbox.

This article is for informational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult qualified healthcare providers for personalized medical guidance.
About Cushion Your Assets:
We understand the frustration of navigating the healthcare system with chronic sitting pain—our founder Trudy Jackson lived it. That's why we created both therapeutic cushions to relieve pressure where it matters most AND a Provider Directory to help you find the specialists who can actually help. We're here to support your entire healing journey.